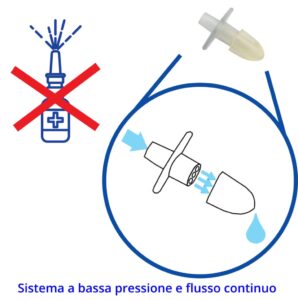
Snoring: new study on nasal dilator Nas-Air®
Internal nasal dilator (Nas-Air®) in patients with snoring
Abstract
Snoring is the most common human habit, which is why it is considered more of a social nuisance than a symptom of a disorder. The nasal valve area corresponds to the smallest cross-section of the upper airway. A problem at this level can easily lead to breathing difficulties and cause snoring. Nasal dilation could therefore significantly improve this disorder. Nas-Air® is a new internal nasal dilator. It was tested in 41 outpatients with snoring. The duration of snoring, assessed using a smartphone, was measured with the Visual Analogue Scale (VAS) for sleep quality perception before and during the use of Nas-Air®. The use of Nas-Air® resulted in a significant reduction in the duration of snoring and an improvement in sleep quality. In conclusion, this study demonstrates that Nas-Air® is an internal nasal dilator capable of reducing the duration of snoring and improving sleep quality.
Keywords: snoring, nasal valve, obstruction, internal nasal dilator, Nas-Air®.
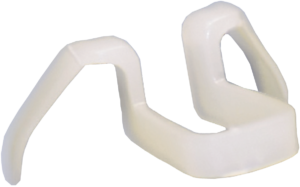
Nas-Air Nasal Dilator
Introduction
Snoring is the most common human habit, which is why it is considered more of a social nuisance than a symptom of a disorder (1). In fact, snoring is prevalent and worsens with age. In young adults, snoring affects 5% of women and 20% of men; in older adults, snoring is present in 40% of women and 60% of men. Furthermore, the importance of nasal obstruction in altering breathing during sleep and wakefulness has long been known. As early as the 19th century, cases of nasal obstruction associated with sleep disorders, insomnia, intellectual deterioration, and memory impairment were reported. Fifty percent of total respiratory resistance is located in the nose, so there is a direct correlation between increased nasal resistance due to nasal obstruction and obstruction of breathing during sleep.
In this context, the nasal valve area has the smallest cross-sectional surface area.
Sleep breathing disorders can be divided into: simple snoring, sleep apnea syndrome, and upper airway resistance syndrome.
The pathogenic mechanisms for snoring are characterized by high-frequency oscillations of the soft palate and pharyngeal walls, epiglottis, and tongue. These oscillations alternately occlude and open the narrow airways. Although the nose is not where the sound is generated, there is evidence to suggest that nasal obstruction may be one of the factors causing sleep-disordered breathing.
Other reports have shown that increasing the patency of the nasal cavity leads to an improvement in snoring (1,6).
The internal nasal valve, which is the shortest portion of the nasal cavity, is formed by the union of the upper lateral cartilages with the nasal septum. The normal angle between these two structures can vary between 10° and 15°. The nasal valve offers greater resistance to airflow in the nose. The smaller the surface area of the site, the more vulnerable it will be to pathological nasal obstruction. Nasal obstruction caused by abnormalities of the nasal valve can be caused by dynamic or static problems and is one of the most important and common causes of nasal obstruction. Despite this, nasal valve collapse is often overlooked as a cause of nasal obstruction. In particular, normal airflow through the nasal valve depends on Bernoulli's principle and Poiseuille's law. Bernoulli's principle states that as airflow through a passage of fixed size increases, the pressure in that space decreases. If the decrease in pressure exceeds the inherent rigidity of the flexible nasal walls, the walls may collapse, resulting in obstruction. From a clinical standpoint, an anatomically narrowed portion of the nasal valve is defined as a static obstruction.
The management of snoring includes careful evaluation and correction of upper airway obstruction. Septoplasty alone, even when combined with lateral osteotomies, did not increase nasal airflow, but correction of a narrowed nasal valve resulted in a 2.5-fold reduction in nasal breathing resistance (2). In fact, even in the presence of a deviated septum, airflow can be improved by restoring a nasal valve obstruction.
It is therefore clear that the assessment and correction of a collapsed nasal valve in a patient with nasal obstruction is essential. Therapeutic methods that increase the area of the nasal valve and reinforce the lateral walls of the nose help to improve nasal patency. Some surgical techniques have proven useful in increasing the area of the nasal valve. Among the most commonly used methods is the use of cartilage grafts. However, mechanical alar nasal dilators may be a potential alternative to surgical procedures. Nasal dilators can be classified as external and internal (3). Many studies have explored the possibility of reducing snoring through the use of these devices.
For these reasons, the aim of this study was to investigate whether the use of a new internal nasal dilator (Nas-Air®) could reduce snoring in a group of outpatients.
Materials and Methods
This study was designed as an open-label study and involved a group of 41 outpatients with snoring.
It was therefore conducted in a real-world setting such as ENT clinics.
I criteri di inclusione prevedevano adulti con episodi di russamento nel mese precedente alla visita. I criteri di esclusione invece erano: gravi problemi anatomici clinici (es. deviazione del setto molto grave e/o ipertrofia dei turbinati, come quella di IV grado), sindrome dell’apnea ostruttiva nel sonno, disturbi e terapie medicinali in corso che potessero potenzialmente interferire con i rilevamenti.
I pazienti sono stati sottoposti a visita otorinolaringoiatrica, con inclusa rinoscopia. Il Nas-Air ® è stato fornito insieme alle corrette istruzioni per l’uso. Tutti i pazienti hanno firmato un consenso informato per la partecipazione allo studio.
In sintesi, il dilatatore nasale interno doveva essere inserito nel naso durante il sonno notturno.
La valutazione del russamento è stata eseguita attraversa l’app “Do I Snore®” via smartphone e registrata a casa durante il sonno. Questa app registra e misura la durata del russamento durante il sonno.
Ai pazienti è stato chiesto di misurare il russamento per due notti (senza Nas-Air ®) e per altre due notti (con Nas-Air ®).
Durante la visita otorinolaringoiatrica sono stati presi in considerazione i seguenti parametri: età, sesso, indice di massa corporea (BMI), Ostruzione della Valvola Nasale, secondo i criteri validati (4), la dimensione dei turbinati, la deviazione del setto e la dimensione delle tonsille.
Alle dimensioni dei turbinati e delle tonsille abbiamo attribuito un valore tra 0 (= dimensione normale) e 4 (=dimensione massima) secondi i criteri validati (5).
I parametri soggettivi sono stati valutati dai pazienti al basale, ad esempio prima di inserire Nas-Air ®. L’ostruzione nasale, la qualità del sonno e dell’olfazione sono stati inclusi e misurati secondo la visual analogue scale (VAS). Il punteggio VAS per l’ostruzione nasale poteva oscillare tra 0 (= naso completamente ostruito) a 10 (= naso completamente libero); il punteggio VAS per l’olfazione poteva oscillare tra 0 (= nessun olfatto) a 10 (= olfatto ottimale); il VAS per la qualità del sonno poteva oscillare tra 0 (= sonno pessimo) a 10 (= sonno ottimo). Inoltre il VAS è stato utilizzato per misurare la soddisfazione dell’uso di Nas-Air ® (0= pessimo; 10= eccellente). Il VAS della qualità del sonno è stato registrato dai pazienti al basale, dopo le due notti senza Nas-Air ®, e dopo le due notti con Nas-Air ®. Sovrappeso/obesità sono stati considerati secondo la definizione WHO come indice di massa corporea > 25 (http://www.who.int/mediacentre/factsheets/fs311/en/ ultimo accesso 29 Marzo 2018).
Le caratteristiche demografiche e cliniche sono state descritte con le medie con DS per i dati a distribuzione normale e con frequenza assoluta e percentuali per categorie variabili. Ogni differenza statistica significativa tra i valori medi di ogni variabile continua sono stati misurati con il t test accoppiato (confronto tra due gruppi) o le misure ripetute ANOVA (confronto tra tre gruppi), seguiti rispettivamente dal Test di confronto multiplo di Bonferroni, come test post-hoc.
Nel caso di frequenze attese inferiori a 5, sono stati utilizzati il test Chi-quadro o il Test esatto di Fisher. Le correlazioni sono state valutate con il coefficiente di correlazione di Pearson. La significatività statistica è stata fissata <0.05, e le analisi sono state effettuate tramite il software GraphPad Prism, GraphPad Software Inc, CA, USA.
Results
L’utilizzo di Nas-Air ® ha significativamente ridotto la durata del russamento (espressa in % russamento durante il sonno) da 36.80 (+ 16.42) % rispettivamente prima dell’applicazione a 23-00 (+ 14.77) (p<0.001) e 23.54 (+ 15.70) (p<0.001) dopo una o due notti di utilizzo di Nas-Air ® (Figura 1).
Non sono state rilevate differenze statisticamente significative tra la percentuale di russamento rilevata durante la prima notte e la seconda notte con Nas-Air ® (p=NS). In aggiunta, la frequenza dei pazienti con russamento ridotto dopo l’utilizzo di Nas-Air ® per una o due notti era simile (p=0.48).
La valutazione dell’apprezzamento di Nas-Air ® mediante VAS ha dimostrato che il dispositivo è ben tollerato, dato un punteggio VAS di 6.32 (2.17). Il punteggio VAS dell’apprezzamento di Nas-Air ® era più alto nei pazienti normopeso rispetto ai pazienti in sovrappeso/obesità con rispettivamente 7.60 (0.56) e 5.90 (0.39) (p<0.0299).
Il punteggio VAS sulla qualità del sonno è migliorato significativamente dopo l’utilizzo di Nas-Air ® con 5.98 (2.54) prima e 7.32 (1.98) dopo l’utilizzo (p = 0.0012) (Figura 2), e moderatamente correlati con il punteggio VAS di apprezzamento di Nas-Air ® (Pearson r = 0.476, p = 0.001) (Figura 3).
Discussion
Snoring can be a serious disturbance to a good social and family life. In fact, in a relationship, it is the non-snoring partner who suffers most from these nocturnal noises.
However, as the years go by, even the snorer becomes aware of their problem, waking up with a dry throat and suffering from drowsiness and fatigue during the day.
From a pathophysiological point of view, the nasal valve area is the narrowest passage in the respiratory tract, causing more than half of the resistance to nasal breathing in a healthy subject.
In this regard, the ratio between the cross-sectional area of the nasal valve and the piriform aperture is 1:1.4. The cross-sectional areas vary within the nasal cavity: in the nasal valve it is approximately 30 mm², in the central portion of the cavity it is 120 mm², and in the nasopharynx it is 150 mm². Following mechanical dilation, nasal airflow can increase by up to 25%; it is interesting to note that this variation is comparable to that observed with the use of nasal decongestants. Indeed, with the dilator, the transverse respiratory area increases further; according to Poiseuille's law for laminar flow (p=l/dn, n=4), a slight increase in diameter (d) and area can significantly reduce pressure (p). Furthermore, thanks to the dilation of the nostrils, intrathoracic pressure can be halved (from 4 to 2 cm of H20). Therefore, less energy is required by the respiratory muscles to inhale the same amount of air.
Upper airway narrowing disorders cause many problems, including adenotonsillar enlargement, tumors, chronic rhinitis, congenital anatomical defects, and so on.
In particular, nasal obstruction is the most common cause of snoring (6). Obstruction of the nasal valve is a crucial factor in the pathogenesis of snoring. Many studies have investigated the role of the nasal valve and its subjective and objective measurement (7,8). However, in clinical practice, the most relevant parameter is the perception of snoring by the partner and/or patient.
From a therapeutic point of view, mechanical dilation of the nasal valve is the best non-surgical approach for snorers. There are many dilators, both internal and external. Many studies have investigated their effectiveness, and in most cases, the outcome has been positive (9-12).
Therefore, this study investigated the effectiveness of a new internal nasal dilator: Nas-Air ®
It is interesting to note that approximately 90% of patients achieved a significant improvement in sleep quality and a significant reduction in the duration of snoring.
However, this study has some limitations, including its open design, the limited number of patients involved, the lack of follow-up, and the absence of validated objective parameters.
Therefore, further studies using a more robust methodology are needed.
In conclusion, this study demonstrates that Nas-Air® is an internal nasal dilator capable of reducing the duration of snoring and improving sleep quality.
Authors
M. Gelardi 1, G. Porro 1, B. Sterlicchio 1, N. Quaranta 1, G. Ciprandi 2
and Italian Study Group on Snoring: T. Candreva, G. Ciancio, A. Ciofalo, M. Colucci, M. Curatolo, A. Guglielmi, L. Ianuzzi, P. Intiglietta, M. Landi, C. Lingua, P. Mola, M. Notargiacomo, P. Pecoraro, G. Pellittieri, L. Pintaldi, M. Tomaiuolo, S. Zizzi.
- Otolaryngology, Basic Medical Sciences, Neuroscience and Sense Organs, University of Bari Aldo Moro, Bari, Italy.
- San Martino General Hospital, Genoa, Italy.
Conflict of interest: none
Bibliography
1) Akcam T, Friedman O, Cook TA. The effect on snoring of structural nasal valve dilation with a butterfly graft. Acta Otolaryngol Head Neck Surg 2004; 130:1313-8
2) Leitzen KP, Brietzle SE, Lindsay RW. Correlation between nasal anatomy and objective sleep apnea severity. Otolaryngol Head Neck Surg 2014; 150:325-31
3) Barrett DM, Casanueva FJ, Cook TA. Management of the nasal valve. Facial Plast Surg Clin N Am 2016; 24:219-34
4) Hamilton GS. The external nasal valve. Facial Plast Surg Clin N Am 2017; 25:179-94
5) Ameli F, Brocchetti F, Tosca MA, Signori A, Ciprandi G. Adenoidal hypertrophy and allergic rhinitis: is there an inverse relationship? Am J Rhinol Allergy 2013; 27(1):e5-10
6) Kiyohara N, Badger C, Tjoa T, Wong B. A comparison of over-the-counter mechanical nasal dilators. JAMA Fac Plast Surg 2016; 18:385-9
7) Varendh M, Andersson M, Bjornsdottir E, Hrubos-Strom H, Johanisson A, Arnadottir ES, et al. Nocturnal obstruction is frequent and reduces sleep quality in patients with obstructive sleep apnea. J Sleep res 2017; 4:1-8
8) Ziai H, Bonaparte JP. Reliability and construct validity of the Ottawa valve collapse scale when assessing external nasal valve collapse. J Otolaryngol Head neck Surg 2018; 47:15
9) Ottaviano G, Ermolao A, Nardello E, Muci F, Favero V, Zaccaria M, et al. Breathing parameters associated with two different external nasal dilator strips in endurance athletes. Auris Nasus Larynx 2017; 44:713-8
10) Floyd EM, Ho S, Patel P, Rosenfeld RM, Gordin E. Systematic review and meta-analysis of studies evaluating functional rhinoplasty outcomes with the NOSE score. Otolaryngol Head Neck Surg 2017; 156:809-15
11) Dinardi RR, Ribeiro de Andrade C, Martins-Costa HC, Ibiapina C. Does the Airmax internal nasal dilator increase peak nasal inspiratory flow (PNIF) in adolescent athletes? Int J Ped Otorhinolaryngol 2016; 84:37-42
12) Salturk Z, Inan M, Kumral TL, Atar Y, Yildirim G, Uyar Y. Efficiency of external nasal dilators in pediatric nasal septal deviation. Int J Ped Otorhinolaryngol 2014; 78:1522-5
translated into Italian by the author,
Received March 29, 2018 – Accepted July 2, 2018
J Biol Regul Homeost Agents.2018 Sep-Oct;32(5):1267-1273
Read also:
-
Nasal irrigations of preschool children (scientific article)
-
Nasal irrigation with Nasir® in children (scientific article)
-
Cystic fibrosis: MUC5B and hypertonic solution (scientific article)